Today, recombinant adeno-associated virus (rAAV) has become the main platform for in vivo gene therapy delivery. The first rAAV gene therapy product, Alipogene Tiparvovec (Glybera) from uniQure, was approved by the European Medicines Agency (EMA) in 2012 for the treatment of lipoprotein lipase deficiency. In 2018, the FDA approved Voretigene neparvovec-rzyl (Luxturna), the first rAAV gene therapy to receive U.S. approval.
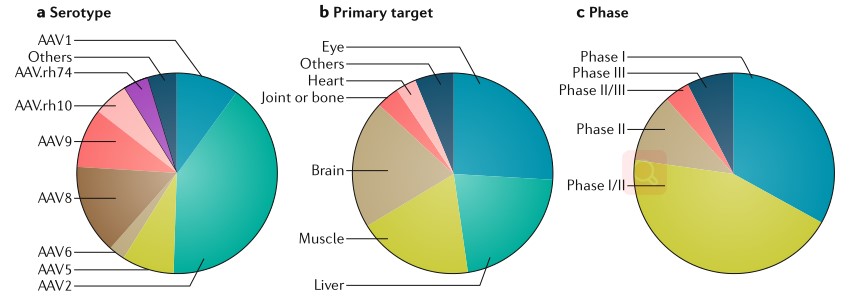 Fig.1 overview of rAAV interventional gene therapy clinical trials.
(Wang, D.; et al. 2019)
Fig.1 overview of rAAV interventional gene therapy clinical trials.
(Wang, D.; et al. 2019)
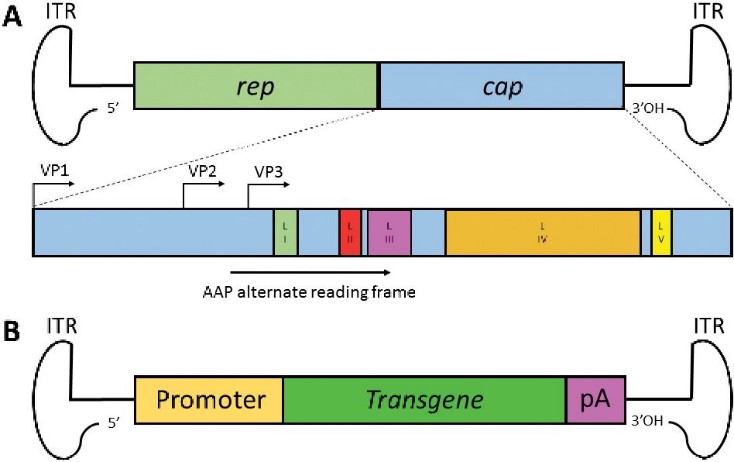
AAV belongs to dependoviruses of the family Parvoviridae and are small, non-enveloped DNA viruses with a genome of about 4.7 kb. AAV vector is a gene delivery tool modified from AAV genome. There is an Inverted terminal repeat (ITR) at both ends of the adeno-associated virus genome, in which the D sequence is closely related to the efficient release, selective replication and packaging of the virus genome. There are two open reading frames in the coding region of the genome. They encode four Rep proteins and three Cap proteins, which play roles in genome replication, viral assembly and packaging, respectively1. When designing AAV vector genome, it is necessary to replace the gene sequence of coding region with the target gene and relevant functional fragment, and only the reverse terminal repeat sequence at both ends is retained. Three plasmid co-transfer method was used in the production, which was to co-transfect cells with plasmid containing AAV vector genome, adenovirus co-gene plasmid, and plasmid expressing CAP and REP proteins. There are currently 13 AAV serotypes (AAV1-AAV13) that target different receptors and tissues. When preparing AAV vectors, different serotypes are usually selected according to the disease site and target tissue.
Therapeutic genes are delivered into designated cells and the dysfunctional genes are replaced by homologous recombination of chromosomes. This technique is suitable for the treatment of recessive single gene hereditary diseases2.
Gene editing technology can directly repair potential disease genes in the human body. It usually involves two steps: targeted DNA disruption and DNA repair to achieve genomic changes.
The AAV vector can participate in the DNA repair process3, deliver the genome with target sequence homologous recombinant arm and therapeutic gene sequence, and finally achieve gene therapy by simultaneous delivery with the gene encoding Cas9 protein.
RNA interference (RNAi) technology occupies the dominant position of rAAV gene silencing platform, which is an important mechanism of mRNA level regulation.
Beyond monogenic diseases, rAAV-mediated gene therapy has the potential to tackle complex genetic diseases and acquired diseases by gene addition. This strategy is currently being tested clinically for HIV infection2.
When an individual is exposed to endogenous AAV infections, an immune response to the AAV capsids can be mounted. Consequently, a percentage of humans express neutralizing antibodies in the blood that could block gene transfer to cellular targets. In addition, administration of recombinant AAVs (rAAVs) can induce antibodies that can neutralize the transduction of AAV gene therapies, activate the innate immune response, and trigger an adaptive immune response that includes a cellular response that may result in loss of transgene expression4.
Sero-epidemiological studies of human wild-type AAV-neutralizing antibodies have shown that the detection rate of anti-AAV2-neutralizing antibodies is highest, ranging from 30% to 60% of the population. Due to extensive cross-reactivity between AAV serotypes, neutralizing antibodies that identify almost all serotypes can be found in subjects5. The main reason is the homology of amino acid sequence and structure between capsids of different AAV serotypes.
In addition to humoral immunity, cellular immunity against AAV1 and AAV2 was also detected by ELISPOT and flow cytometry6. These AAV-specific T cells are highly cross-reactive to different serotypes and are more prevalent in peripheral immune organs of the spleen than in peripheral blood. Most AAV-specific T cells have a memory phenotype and are detected at similar levels in adults and children.
Innate immunity: The AAV vector lacks the sequence encoding the virus, and the main antigenicity comes from the residual contaminants in the purification and production process, viral capsid and transduction gene products, etc. The nucleic acid component of the viral carrier may have an adjuvant-like effect to help activate the host immune system. Through pathogen-associated molecular patterns (PAMP), antigens expressed in viral vectors can be recognized by immune cells' PRR (pattern recognition receptor) to initiate natural immunity. These PRRS can recognize viral nucleic acids, as well as membrane glycoproteins and even chemical messengers. PRR involvement mainly leads to the activation of NF-KB and IRF transcription factors, which play a central role in inducing the expression of pro-inflammatory cytokines or type I IFN, respectively7.
Adaptive immunity: Adaptive immunity occurs after innate immunity by eliminating pathogens through antigen-specific recognition and then establishing immune memory. In establishing an adaptive response, T and B lymphocytes are activated in recognition of the antigen presented by APC. Upon activation, lymphocytes expand and differentiate into effector cells and mediate antigen elimination by inducing humoral immunity or cytotoxic responses. After antigen clearance, memory T and B lymphocytes will be reactivated upon re-exposure to the antigen. It has been demonstrated that gene transfected cells and specialized APCs deliver capsid protein epitopes to cytotoxic CD8+T cells via MHCI-like molecules. Cytotoxic T cells clear AAV transduction cells, leading to inflammation in target organs and reducing the duration and effectiveness of gene transfer. In synchronization with MHCI-class transmission, recognition of capsid derived epitopes on APC surface that bind MHCI-class can activate CD4+T helper cells and promote humoral and cell-mediated immune responses. Clinical trials have shown that the immunogenicity of AAV vectors is to some extent dose-dependent, with low doses of AAV vectors more likely to cause mild inflammation and not a complete loss of transgenic expression8.
During AAV gene transfer, many factors affect the immunogenicity of transgenic products. These can be divided into host-specific factors, associated with the underlying disease or the genetic background of the vector recipient, and vector-specific factors, to group factors related to gene transfer. One key factor determining the level of anti-transgene immune responses is the target organ for gene transfer, which is determined by the combination of the AAV capsid, the vector delivery route, and the tissue specificity of the promoter driving gene expression. In particular, systemic and intramuscular vector administration, with either ubiquitous or muscle-specific promoters, have been shown to be more immunogenic than gene transfer to immune privileged organs, as well as systemic administration with liver-specific promoters9.
Although several AVV vector-based gene therapy drugs are currently approved, the immunogenicity of AVV vectors remains an important barrier to their use, both in preclinical and clinical studies. For example, human and non-human primates exposed to wild-type AAV typically carry anti-capsid neutralizing antibodies (NAbs) that cross-react with several different serotypes used for gene transfer. After vector inoculation, the anti-AAV NAb rapidly develops a high titer that persists for several years, preventing vector re-administration.
The clear definition of the baseline immunological parameters of gene transfer is therefore important to ensure accurate results interpretation in both preclinical and clinical studies. Methods for detecting AAV immunity include cell-based TI tests in vitro, TI tests in vivo (e.g., mice), and total anti-capsid antibody (TAb) tests based on enzyme linked immunosorbent assay10 (ELISA). TAb method may be able to detect low-efficiency NAb below the TI detection threshold, but it may not detect non-antibody neutralizing factors. In vivo and in vitro, TI tests screened samples for anti-AAV, NAb, and other factors that regulate AAV transduction efficiency.
Creative Diagnostics offers a comprehensive selection of adeno-associated virus (AAV) antibodies, which can proficiently identify complete virus capsids. Moreover, we provide antibodies that are tailored to AA-viral subunits and replicases. Additionally, we have titration ELISA kits for diverse AAV subtypes at your disposal.
Anti-AAV Antibody ELISA Kit
AAV Antibodies and Titration ELISA
References
| Cat. | Product Name | Host | Specificity | |
| DMAB6350 | Anti-AAV1 (intact particle) Mab, clone BEL2b | Mouse | Reacts with AAV1, AAV6, AAV12 intact capsids, empty and full capsids. | Inquiry |
| DMAB-CS24040 | Magic™ Anti-AAV2 (intact particle) Mab, clone 26H5 | Rabbit | Recognizes a conformational epitope on AAV2. No cross-reaction with AAV type 1, 5, 6, 8, 9, DJ, rh.1 in Dot Blot. AAV3, AAV4, AAV7 and AAV10 are not tested. | Inquiry |
| DMAB-CS24041 | Magic™ Anti-AAV2 (intact particle) Mab, clone 44H6 | Rabbit | Recognizes a conformational epitope on AAV2. No cross-reaction with AAV type 1, 5, 6, 8, 9, DJ, rh.1 in Dot Blot. AAV3, AAV4, AAV7 and AAV10 are not tested. | Inquiry |
| CABT-B9062 | Anti-AAV2 (intact particle) Mab, clone B31 | Mouse | Reacts with AAV2, AAV2 7m8 and AAV3 intact particles, empty and full capsids. | Inquiry |
| CABT-LY428 | Anti-AAV2 (intact particle) Mab, clone B31 | Mouse | Reacts with AAV2, AAV2 7m8 and AAV3 intact particles, empty and full capsids. | Inquiry |
| CABT-R9062L | Anti-AAV2 (intact particle) Mab, clone B31 | Humanized | Reacts with AAV2, AAV2 7m8 and AAV3 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24227 | Anti-AAV2 (intact particle) Mab, clone B31 | Canine | Reacts with AAV2, AAV2 7m8 and AAV3 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24228 | Anti-AAV2 (intact particle) Mab, clone B31 | Rat | Reacts with AAV2, AAV2 7m8 and AAV3 intact particles, empty and full capsids. | Inquiry |
| DMAB6352 | Anti-AAV4 (intact particle) Mab, clone BEL5 | Mouse | Reacts with AAV4 intact particles, empty and full capsids. | Inquiry |
| DMAB6353 | Anti-AAV5 (intact particle) Mab, clone BEL6b | Mouse | Reacts with AAV5 intact capsids, empty and full capsids. | Inquiry |
| DMAB6354 | Anti-AAV5 (intact particle) Mab, clone BEL6c | Mouse | Reacts with AAV5 intact capsids, empty and full capsids. | Inquiry |
| DMAB-CS23065 | Anti-AAV5 (intact particle) Mab, clone F56 | Humanized | Reacts with AAV5 intact capsids, empty and full capsids. | Inquiry |
| DMAB-CS24200 | Anti-AAV5 (intact particle) Mab, clone Y506 | Canine | Reacts with AAV5 intact capsids, empty and full capsids. | Inquiry |
| DMAB-CS24229 | Anti-AAV5 (intact particle) Mab, clone BEL6b | Rat | Reacts with AAV5 intact capsids, empty and full capsids. | Inquiry |
| CABT-B9064 | Anti-AAV6 (intact particle) Mab, clone BEL7 | Mouse | Reacts with AAV6 intact particles, empty and full capsids. | Inquiry |
| CABT-R9064L | Anti-AAV6 (intact particle) Mab, clone BEL7 | Humanized | Reacts with AAV6 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24230 | Anti-AAV6 (intact particle) Mab, clone BEL7 | Canine | Reacts with AAV6 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24231 | Anti-AAV6 (intact particle) Mab, clone BEL7 | Rat | Reacts with AAV6 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24042 | Magic™ Anti-AAV8 (intact particle) Mab, clone 86F3 | Rabbit | Recognizes a conformational epitope on AAV8. No cross-reaction with AAV type 1, 2, 5, 6, 9, DJ, rh.1 in Dot Blot. AAV3, AAV4, AAV7 and AAV10 are not tested. | Inquiry |
| DMAB-CS24043 | Magic™ Anti-AAV8 (intact particle) Mab, clone 83F9 | Rabbit | Recognizes a conformational epitope on AAV8. No cross-reaction with AAV type 1, 2, 5, 6, 9, DJ, rh.1 in Dot Blot. AAV3, AAV4, AAV7 and AAV10 are not tested. | Inquiry |
| CABT-B9065 | Anti-AAV8 (intact particle) Mab, clone BEL9 | Mouse | Reacts with AAV3, AAV7, AAV8, AAVrh10, AAVrh74 and Anc80 intact particles, empty and full capsids. | Inquiry |
| CABT-LY254 | Anti-AAV8 (intact particle) Mab, clone BEL9 | Humanized | Reacts with AAV3, AAV7, AAV8, AAVrh10, AAVrh74 and Anc80 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24232 | Anti-AAV8 (intact particle) Mab, clone BEL9 | Canine | Reacts with AAV3, AAV7, AAV8, AAVrh10, AAVrh74 and Anc80 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24233 | Anti-AAV8 (intact particle) Mab, clone BEL9 | Rat | Reacts with AAV3, AAV7, AAV8, AAVrh10, AAVrh74 and Anc80 intact particles, empty and full capsids. | Inquiry |
| CABT-B9066 | Anti-AAV8/9 (intact particle) Mab, clone BEL9/0 | Mouse | Reacts with AAV8, AAVrh10, Anc80 and AAVrh74 intact particles, empty and full capsids. Weak affinity for AAV9 and AAVDJ intact particles. | Inquiry |
| DPAB-AV01 | Anti-AAV9 (intact particles) Mab, clone BEL0 | Mouse | Reacts with AAV9 intact particles, empty and full capsids. | Inquiry |
| CABT-L6458Z | Anti-AAV9 (intact particle) Mab, clone BEL0 | Mouse | Reacts with AAV9 intact particles, empty and full capsids. | Inquiry |
| CABT-L21Y197 | Anti-AAV9 (intact particle) Mab, clone BEL0 | Human | Reacts with AAV9 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24199 | Anti-AAV9 (intact particle) Mab, clone Y505 | Canine | Reacts with AAV9 intact particles, empty and full capsids. | Inquiry |
| DMAB-CS24234 | Anti-AAV9 (intact particle) Mab, clone BEL0 | Rat | Reacts with AAV9 intact particles, empty and full capsids. | Inquiry |
| DMAB6345 | Anti-AAV2 Replicase Mab, clone A304.10 | Mouse | Reacts with AAV2 Rep40, Rep52, Rep68 and Rep78. | Inquiry |
| DMAB6346 | Anti-AAV2 Replicase Mab, clone A227.8 | Mouse | Reacts with AAV2 Rep40, Rep52, Rep68 and Rep78. | Inquiry |
| DMAB6347 | Anti-AAV2 Replicase Mab, clone A77.4 | Mouse | Reacts with AAV2 Rep52 and Rep78. | Inquiry |
| DMAB6348 | Anti-AAV2 VP1 Mab, clone B2 | Mouse | Reacts with VP1 of AAV1, AAV2, AAV3, AAV5, AAV6, AAV7, AAV8, AAV9 and AAVDJ. Epitope mapping experiments identified aa123 to aa131 of VP1 capsid protein as the specific binding region. | Inquiry |
| DMAB-CS24045 | Anti-AAV VP1 Mab, clone 25G6 | Rabbit | Reacts with VP1 of AAV1, AAV2, AAV6, AAV8, AAV9, AAVDJ. It does not react with AAV5 and AAVrh.1. AAV3, AAV4, AAV7 and AAV10 are not tested. | Inquiry |
| DMAB6349 | Anti-AAV2 VP1/VP2 Mab, clone B610 | Mouse | Reacts with VP1 and VP2 of AAV2 and AAVDJ. Epitope mapping experiments identified aa169 to aa184 of VP2 and (with reduced intensity) aa123 to aa136 of VP1 capsid proteins as the specific binding region. | Inquiry |
| DMAB2922 | Anti-AAV VP1/VP2/VP3 Mab, clone B2 | Mouse | Reacts with denatured VP1, VP2, VP3 proteins of AAV1, 2, 3, 5, 6, 7, 8, 9, rh10, DJ. Epitope mapping experiments identified aa726 to aa733 (C-terminus; common to all 3 VP proteins) as the specific binding region. | Inquiry |
| DPAB2423 | Anti-AAV2 VP1/VP2/VP3 Pab | Rabbit | Reacts with denatured proteins VP1, VP2, and VP3 of AAV1, AAV2, AAV3, AAV5, AAV6, AAV7, AAV8, AAV9, AAVrh10, AAVDJ and AAVrh74, weakly with AAV4. It detects native capsids with significantly lower affinity. | Inquiry |
| DPAB2424 | Anti-AAV5 Pab | Rabbit | Reacts with virus capsid proteins VP1, VP2, VP3 of AAV5; no cross-reaction with AAV types 1 - 4. | Inquiry |
| Cat. | Product Name | Serotype | |
| DAG-WT823 | Recombinant Adeno-associated Virus Type 1 (AAV1) VLP | AAV1 | Inquiry |
| DAG-WT824 | Recombinant Adeno-associated Virus Type 2 (AAV2) VLP | AAV2 | Inquiry |
| DAG-WT825 | Recombinant Adeno-associated Virus Type 5 (AAV5) VLP | AAV5 | Inquiry |
| DAG-WT826 | Recombinant Adeno-associated Virus Type 8 (AAV8) VLP | AAV8 | Inquiry |
| DAG-WT827 | Recombinant Adeno-associated Virus Type 9 (AAV9) VLP | AAV9 | Inquiry |
| DAGC255 | AAV1 capsids (ELISA Control) | AAV1 | Inquiry |
| DAGC256 | AAV2 capsids (ELISA Control) | AAV2 | Inquiry |
| DAGC257 | AAV5 capsids (ELISA Control) | AAV5 | Inquiry |
| DAGC258 | AAV6 capsids (ELISA Control) | AAV6 | Inquiry |
| DAGC259 | AAV8 capsids (ELISA Control) | AAV8 | Inquiry |
| DAGC521 | AAV9 capsids (ELISA Control) | AAV9 | Inquiry |
| Cat. | Product Name | Application | |
| DEIASL345 | Human Anti-AAV8 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL345M | Mouse Anti-AAV8 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL348 | Human Anti-AAV9 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL348M | Mouse Anti-AAV9 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL347 | Human Anti-AAV2 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL344 | Human Anti-AAV6 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
| DEIASL343 | Human Anti-AAV5 Antibody ELISA Kit | Qualitative ELISA | Inquiry |
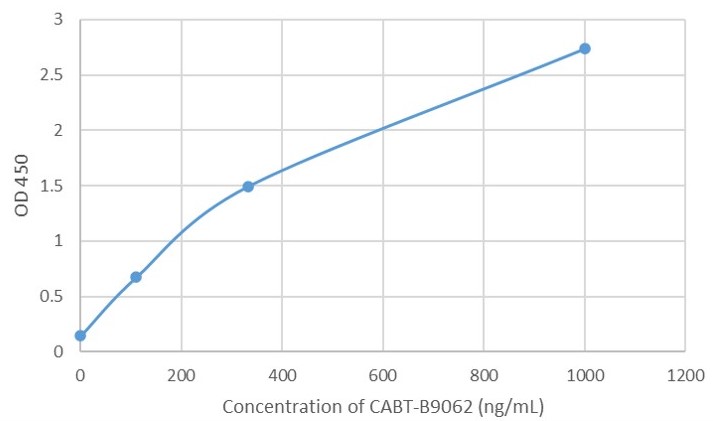
a
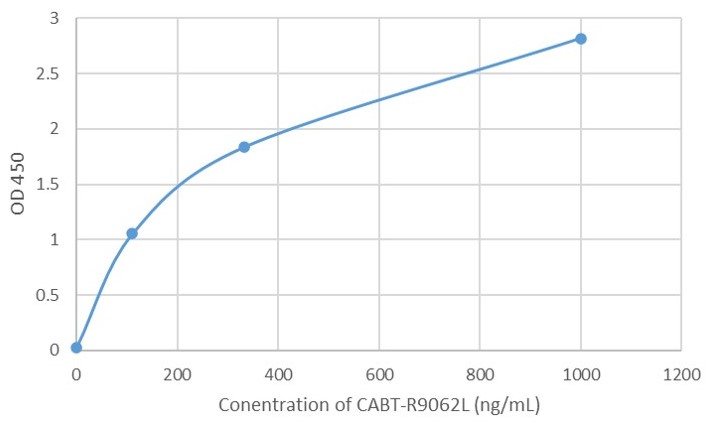
b
c
d
e
f
g
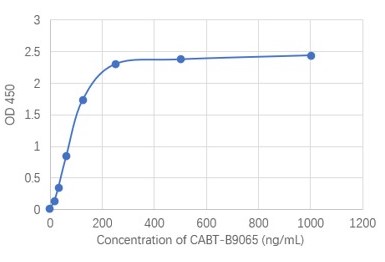
h
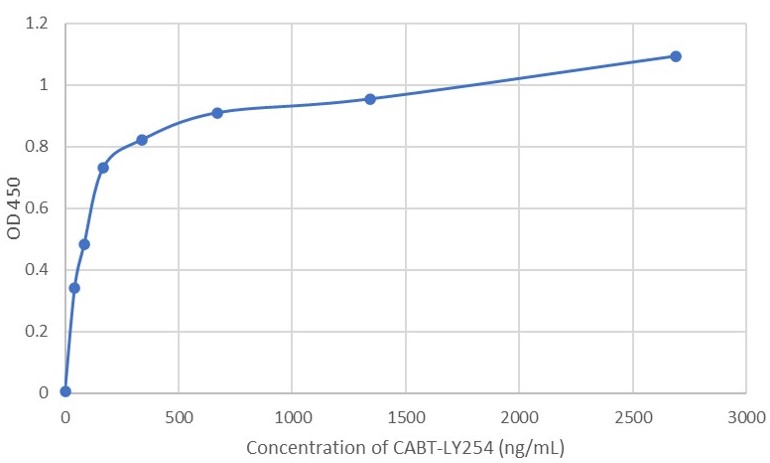
i
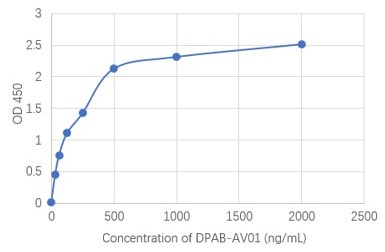
j
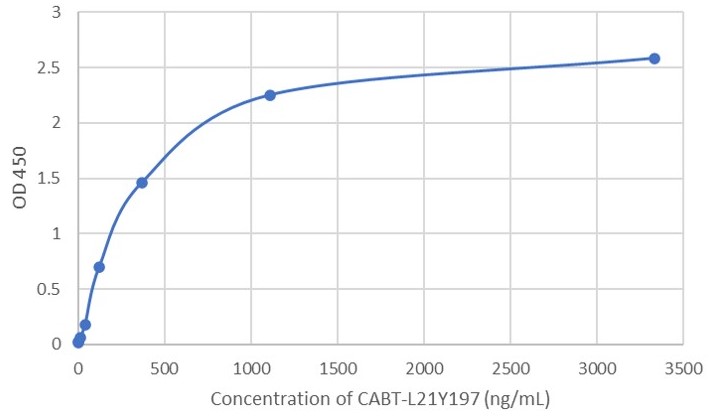
k
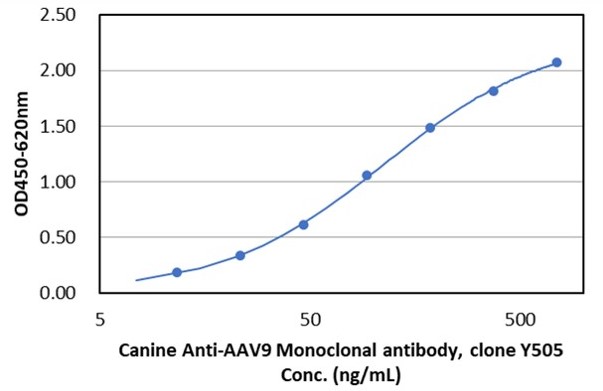
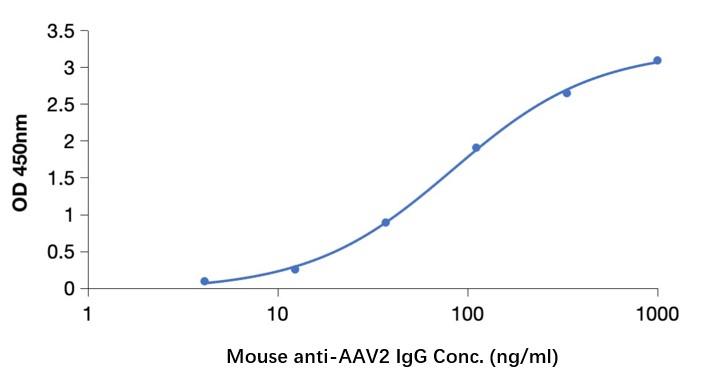
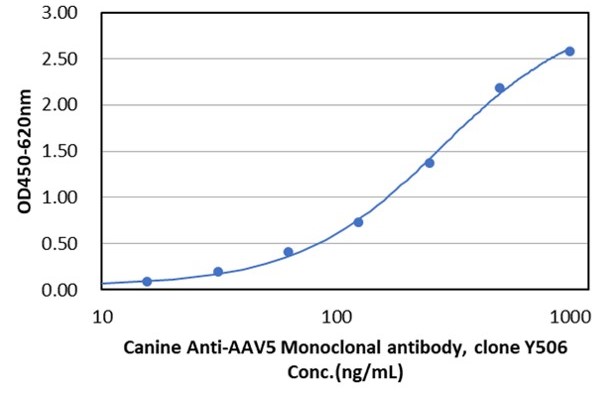
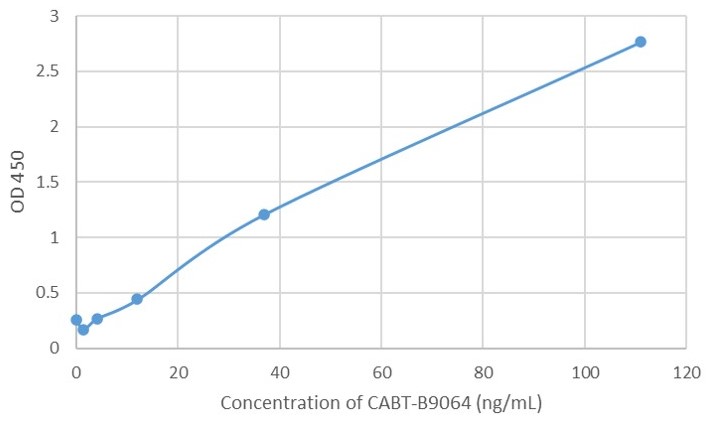
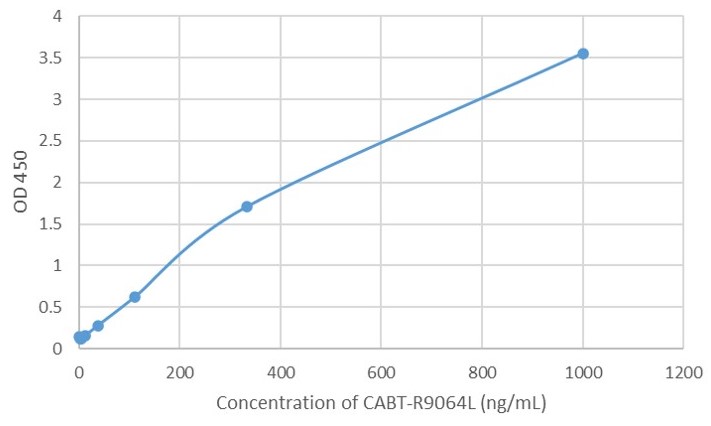
Fig. 1 AAV intact particle Mabs activity detection by Indirect ELISA
a: AAV2 Mouse Mab (CABT-B9062).
d: AAV5 Canine Mab (DMAB-CS24200).
g: AAV8 Mouse Mab (CABT-B9065).
j: AAV9 Human Mab (CABT-L21Y197),
b: AAV2 Human Mab (CABT-R9062L).
e: AAV6 Mouse Mab (CABT-B9064).
h: AAV8 Human Mab (CABT-LY254).
k: AAV9 Canine Mab (DMAB-CS24199).
c: AAV2 Mouse Mab (CABT-LY428).
f: AAV6 Human Mab (CABT-R9064L).
i: AAV9 Mouse Mab (DPAB-AV01).